Introduction
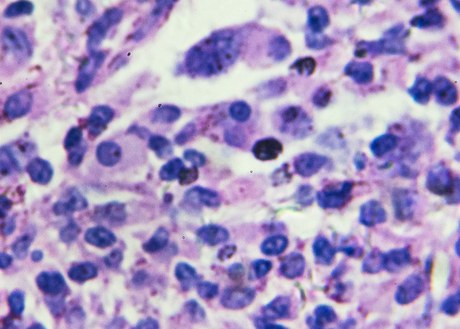
Mantle cell lymphoma (MCL) is a heterogenous non-Hodgkin B-cell lymphoma that can be aggressive, difficult to treat, and often yields poor outcomes in advanced stages. Advances in treatment for MCL have significantly improved outcomes in the last two decades. Intensive induction regimens consisting of cytarabine and rituximab followed by autologous stem cell transplant (ASCT) in first complete remission (CR) have led to improvements in overall survival (OS) rates from 5 years to 11-12 years.1-3 Despite this, optimal first-line treatment of MCL is still debated as relapse is common in this heterogenous disease, especially in high-risk patients, often defined as those with TP53 alterations, Ki-67 >30%, and/or blastoid morphology.4 Recent advances in the front-line space have questioned the role of ASCT and introduced targeted therapies such as Bruton tyrosine kinase inhibitors (BTKis) which were previously reserved for second line.
Outcomes of induction chemotherapy followed by autologous transplant
The benefit of ASCT after first-line chemotherapy in MCL was demonstrated in a landmark randomized controlled trial (RCT) by the European Mantle Cell Lymphoma Network that compared the efficacy and safety of ASCT versus interferon alfa maintenance.5 Induction chemotherapy most often consisted of cyclophosphamide, doxorubicin, vincristine, and prednisone (CHOP), but patients could receive rituximab plus CHOP (R-CHOP) or CHOP-like regimens. The original study demonstrated improved progression-free survival (PFS) with ASCT but did not have enough power to detect a difference in OS. A long-term study with a median follow-up of 14 years examined OS and explored whether the addition of rituximab to first-line induction affected these outcomes.6 As shown in Table 1, median PFS and OS were higher in the ASCT group; however, for patients treated with rituximab, this statistically significant PFS and OS benefit was not seen. This analysis demonstrated that additional data is needed to examine the value of ASCT in the rituximab era.
Since this study, there have been further advances in first-line therapy such as improvements in induction regimens to include cytarabine as well as the implementation of rituximab maintenance (RM). The MCL Younger trial compared R-CHOP alternating with rituximab plus dexamethasone, high-dose cytarabine, and cisplatin (R-DHAP) followed by ASCT versus R-CHOP and ASCT.3,7 With a median follow-up of 6.1 years, the original report demonstrated a longer time to treatment failure (TTF) in the R-DHAP arm but not a statistically significant difference in OS. Longer term follow up demonstrated a significant OS benefit when adjusting for higher risk disease.
Other cytarabine-based regimens have been evaluated in single-arm studies and support optimization of induction regimens with cytarabine. In the 15-year follow-up of the Nordic MCL2 study, median PFS was 8.5 years, and median OS was 12.7 years.8 This regimen included Maxi-CHOP for 3 cycles alternating with high-dose cytarabine for 3 cycles and incorporated rituximab. After ASCT, patients also received a preemptive course of weekly rituximab in the event of positive minimal residual disease (MRD), a test used to detect remaining cancer cells not apparent on imaging.9
The LYMA study demonstrated the benefit of RM after ASCT.10 Patients initially received 4 courses of R-DHAP, and in the event of a partial response (PR), 4 cycles of R-CHOP were given. After ASCT, patients were randomized to receive RM at a dose of 375 mg/m2 every 2 months for 3 years or observation. MRD status did not influence maintenance assignment. At 4 years, the primary endpoint of event-free survival (EFS) as well as PFS and OS were all superior for the RM arm. In a long-term follow-up study, EFS and PFS were prolonged at 7 years, but a statistically significant benefit was not shown for OS.11
| Trial | Regimen | Patients | Outcomes |
| European MCL Network | CHOP, R-CHOP, or CHOP-like regimen followed by ASCT vs interferon alfa maintenance | 269 patients aged < 66 | • Median PFS: 3.3 years vs 1.5 years (P<0.001) |
| • Median OS: 7.5 years vs 4.8 years (P=0.19) | |||
| • Median PFS for patients treated with rituximab: 3.4 years vs 1.7 years (P=0.087) | |||
| • Median OS for patients treated with rituximab: 9.6 years vs 5.5 years (P=0.68) | |||
| MCL Younger | R-CHOP/R-DHAP + ASCT vs R-CHOP + ASCT | 497 patients aged < 66 | • Median TTF: 8.4 years vs 3.9 years (P=0.038) |
| • Median OS: NR vs 11.3 years (P=0.12) | |||
| Nordic MCL2 | R-maxi-CHOP/HIDAC + ASCT | 160 patients aged < 66 | • Median PFS: 8.5 years |
| • Median OS: 12.7 years | |||
| LYMA | R-DHAP* + ASCT followed by RM or observation | 240 patients aged < 66 | • EFS at 4 years: 79% vs 61% (P=0.001) |
| • PFS at 4 years: 83% vs 64% (P<0.001) | |||
| • OS at 4 years: 89% vs 80% (P= 0.002) | |||
| • Median EFS at 7 years: NR vs 5.8 years (P<0.0001) | |||
| • PFS at 7 years: 78.5% vs 47.4% (P<0.0001) | |||
| • OS at 7 years: 83.2% vs 72.2% (P=0.088) |
CHOP, cyclophosphamide, doxorubicin, vincristine, prednisone; R-CHOP, rituximab, cyclophosphamide, doxorubicin, vincristine, prednisone; ASCT, autologous stem cell transplantation; PFS, progression free survival; OS, overall survival; R-DHAP, rituximab, dexamethasone, high-dose cytarabine, cisplatin; TTF, time to treatment failure; NR, not reached; HIDAC, high-dose cytarabine; BR, bendamustine, rituximab; RC, rituximab, high-dose cytarabine; RM, rituximab maintenance; EFS, event free survival
*Cisplatin could be submitted with oxaliplatin or carboplatin, and 4 cycles of R-CHOP were given if partial response
Outcomes of newer BTKi based first-line regimens
BTK inhibition has been a key target in the treatment of relapsed and refractory MCL. Recent trial data in the first-line suggests an earlier role for BTKis. Expert guidance recommends BTKi based regimens in the first-line for all stages of disease including TP53 mutated disease based on compelling evidence.12
The TRIANGLE study demonstrated the benefit of adding BTKi to first-line therapy with significantly improved failure free survival (FFS) when adding ibrutinib to alternating cycles of R-CHOP and R-DHAP followed by ASCT compared to ASCT alone (Table 2).13 There was comparable toxicity with this addition during induction and ASCT but an increase in grade 3-5 hematological adverse events and infections during maintenance and follow-up. While results are still ongoing for one arm of the trial directly comparing BTKi without ASCT to ASCT without BTKi, the superior efficacy of the addition of BTKi to front line therapy especially in younger patients highlighted the importance of targeted therapy in this setting regardless of transplant.
The ECHO study also found benefit in adding BTKi to a front line less intensive induction regimen.14 In patients ≥65 years, acalabrutinib was added to six cycles of BR, a regimen typically reserved for those not suitable for more aggressive induction therapy, followed by RM for 2 years. MRD was assessed at screening, every 24 weeks, and at progression or complete response. The addition of BTKi led to a significant improvement in PFS and MRD-negativity with little difference in toxicity. This is in spite of results of the SHINE trial that showed an improvement in median PFS but an increase in deaths when adding ibrutinib to BR likely due to a worse toxicity profile of ibrutinib compared to newer generation BTKis.15 An updated analysis of ECHO after 50 months confirmed these results, including a longer time to next treatment in the BTKi arm.16
In a similar study by Jain and colleagues aimed at older, frailer patients with MCL, a study of acalabrutinib in addition to rituximab alone found promising results as a potential chemotherapy-free regimen and included higher risk patients such as those with TP53 positive and blastoid morphology.17
A phase II study of zanubrutinib, obinutuzumab, and venetoclax (BOVen) in TP53 positive MCL patients found promising efficacy from a targeted therapy approach to first-line treatment in a high-risk patient population.18 While it only included 25 patients, the positive results of a targeted approach compared to poor survival outcomes typically seen with more intensive chemoimmunotherapy provide evidence for a change in treatment standards for this heterogenous disease.
Table 2. Clinical trials investigating BTKi use in first-line treatment of MCL 13-18
| Trial | Regimen | Patients | Outcomes |
| TRIANGLE | Group A (RCHOP alternating with R-DHAP followed by ASCT) | 870 patients age < 66 years | • 3-year failure free survival |
| Group A + I (addition of ibrutinib on days 1-9 of RCHOP cycles and maintenance for 2 years) | - A+I vs A (superiority) 88% (95% CI 84-92) vs (72% (95% CI 67-79); HR 0.52, p = 0.0008 | ||
| - A vs I (nonsuperiority) 72% (95% CI 67-79) vs 86% (95% CI 82-91); HR 1.77, p = 0.9979 | |||
| Group I (addition of ibrutinib as above, ASCT was omitted) | - A+I vs I ongoing | ||
| ECHO | Acalabrutinib or placebo + BR | 598 patients age ≥ 65 years | • Median PFS: 66.4 mo (acalabrutinib) vs 49.6 mo (placebo); HR 0.73 (95% CI 0.57-0.94), p = 0.0160 |
| • Median time to next treatment: NR (acalabrutinib) vs 73.8 mo (placebo) | |||
| • Conversion to MRD-negative during maintenance phase: 37.5% (acalabrutinib) vs 20% (placebo) | |||
| SHINE | Ibrutinib or placebo + BR | 523 patients age ≥ 65 years | • Median PFS 80.6 mo (ibrutinib) vs 52.9 mo (placebo); HR 0.75 (95% CI 0.59-0.96, p = 0.01) |
| Jain, et al | Acalabrutinib plus rituximab weekly x4 weeks, followed by once a month for 12 months, once every 2 months for 24 total months | 50 patients age ≥ 65 years | • ORR 94% |
| • CRR 90% | |||
| • MRD negativity 14/28 | |||
| • At 17 months, median PFS: NR; OS: NR | |||
| BOVen | Fixed duration of 24 cycles: Zanubrutinib, obinutuzumab cycles 1-8, venetoclax ramp up after 2 cycles | 25 patients, adults median age 68 years (range, 29-82) | • ORR 96% |
| • CRR 88% | |||
| • Undetectable MRD after 24 cycles at a sensitivity level of 1 x 10-5: 95% | |||
| • 2-year PFS: 72%, OS: 76% |
R-CHOP, rituximab, cyclophosphamide, doxorubicin, vincristine, prednisone; R-DHAP, rituximab, dexamethasone, high-dose cytarabine, cisplatin or oxaliplatin; ASCT, autologous stem cell transplantation; HR, hazard ratio; BR, bendamustine, rituximab; PFS, progression free survival; ORR, overall response rate; CRR, complete response rate; MRD, minimal residual disease; NR, not reached; OS, overall survival
Discussion
Optimizing treatment for MCL in the first-line is crucial for improved outcomes as time to progression and survival are shorter with each subsequent line of treatment.19 Traditional chemoimmunotherapy, ASCT, and RM have significantly improved outcomes in the last decade although recent studies have questioned this historical standard. While the addition of BTKi therapy in the first-line setting and the utilization of MRD monitoring has further challenged preferred initial treatment in MCL through providing impactful options for older patients, the addition of BTKi into the first-line setting and whether it eliminates the need for ASCT remains a subject of debate.
In the absence of RCTs evaluating ASCT with cytarabine-based regimens and RM, retrospective data has been conflicting. The North American Mantle Cell Lymphoma Project involved 23 institutions seeking to update prognostic models for MCL.20 This retrospective study included 586 MCL cases diagnosed between 2000 and 2021, and 33% of these patients received stem cell transplant (SCT) (80% autologous and 20% allogeneic). Of all the parameters evaluated, SCT had the most significant impact on PFS and OS. Though 20% received RM, improvements in PFS and OS were only significant in the total cohort and older cohort. Cytarabine-based regimens and SCT improved PFS in younger patients. Based on these results, the authors of this study concluded that ASCT, clinical trials, and RM should be recommended in high-risk patients.
In contrast, a few more recent studies have demonstrated a lack of benefit of ASCT. A retrospective trial using the Flatiron Health database included 4,216 patients diagnosed between 2011 and 2021 and mostly treated in community oncology settings.21 Of the 1,265 patients under 65 years, 23.5% received ASCT, and ASCT was not significantly associated with increases in real world time to next treatment (rwTTNT) (P=0.1) or OS (P=0.4). Three-year OS was 88% for those who received ASCT and 84% for those who did not, and 3-year rwTTNT was 65% versus 59%. Similarly, the validation cohort of academic centers did not show an improvement in outcomes with ASCT.
Further, the emergence of MRD testing has allowed for better understanding of disease burden and risk of relapse following induction treatment which may help guide patient populations who would benefit from ASCT. MRD was utilized in more recently published literature including but not limited to the ECHO study, BOVen, and ECOG-ACRIN EA4151.
Interim results of ECOG-ACRIN EA4151 address the role of ASCT in patients with undetectable MRD.22 Patients were randomized to ASCT and 3 years of RM or maintenance alone for 3 years if in CR with undetectable MRD at 1 in 10-6 sensitivity. In the case of MRD positive CR or MRD indeterminate, patients received both ASCT and RM. For the patients who received ASCT and maintenance, 3-year OS was 82.1%, and 3-year OS was 82.7% for the patients who received RM alone. Three-year PFS was 76.6% for the ASCT and RM group and 77.4% for RM alone. Thus, patients with undetectable MRD in first CR did not have improved outcomes with ASCT. Still, these results do not clarify the optimal strategy for ASCT or maintenance in patients who remain MRD positive after initial therapy since those patients received both treatments.
Together with the ECOG-ACRIN EA4151 study, the TRIANGLE study supports an emphasis on maintenance over ASCT consolidation in transplant-eligible patients, implementing ibrutinib maintenance but also optional RM. However, this data leads to additional questions around optimization of maintenance strategies and subsequent therapy. Since ibrutinib use is off-label for MCL in the United States and since it has a greater side-effect burden, substitution with a 2nd generation BTKi is desirable. Additionally, utilization of BTKis in first-line brings into question the utility of re-exposure to BTKis in the second line. The TRIANGLE study employed a fixed 2-year duration of BTKi maintenance, suggesting re-exposure in relapse could induce further responses although data remains limited.13
In conclusion, recent data suggests that ASCT may not be necessary for all patients. Rather, maintenance for patients with negative MRD and BTKi incorporation into initial therapy and maintenance have demonstrated positive outcomes and continue to be explored. Given this emerging literature and follow-up from previously published data, future studies in this heterogenous disease can help guide BTKi sequencing and populations best suited for less intensive chemotherapy-containing regimens vs ASCT upfront.
References
-
Herrmann A, Hoster E, Zwingers T, et al. Improvement of Overall Survival in Advanced Stage Mantle Cell Lymphoma. J Clin Oncol. 2009;27(4):511-518. doi:10.1200/JCO.2008.16.8435
-
Eskelund CW, Kolstad A, Jerkeman M, et al. 15-year follow-up of the Second Nordic Mantle Cell Lymphoma trial (MCL2): prolonged remissions without survival plateau. Br J Haematol. 2016;175(3):410-418. doi:10.1111/bjh.14241
-
Hermine O, Jiang L, Walewski J, et al. High-Dose Cytarabine and Autologous Stem-Cell Transplantation in Mantle Cell Lymphoma: Long-Term Follow-Up of the Randomized Mantle Cell Lymphoma Younger Trial of the European Mantle Cell Lymphoma Network. J Clin Oncol. 2023;41(3):479-484. doi:10.1200/JCO.22.01780
-
Scheubeck G, Jiang L, Hermine O, et al. Clinical outcome of Mantle Cell Lymphoma patients with high-risk disease (high-risk MIPI-c or high p53 expression). Leukemia. 2023;37(9):1887-1894. doi:10.1038/s41375-023-01977-y
-
Dreyling M. Early consolidation by myeloablative radiochemotherapy followed by autologous stem cell transplantation in first remission significantly prolongs progression-free survival in mantle-cell lymphoma: results of a prospective randomized trial of the European MCL Network. Blood. 2005;105(7):2677-2684. doi:10.1182/blood-2004-10-3883
-
Zoellner AK, Unterhalt M, Stilgenbauer S, et al. Long-term survival of patients with mantle cell lymphoma after autologous haematopoietic stem-cell transplantation in first remission: a post-hoc analysis of an open-label, multicentre, randomised, phase 3 trial. The Lancet Haematology. 2021;8(9):e648-e657. doi:10.1016/S2352-3026(21)00195-2
-
Hermine O, Hoster E, Walewski J, et al. Addition of high-dose cytarabine to immunochemotherapy before autologous stem-cell transplantation in patients aged 65 years or younger with mantle cell lymphoma (MCL Younger): a randomised, open-label, phase 3 trial of the European Mantle Cell Lymphoma Network. The Lancet. 2016;388(10044):565-575. doi:10.1016/S0140-6736(16)00739-X
-
Eskelund CW, Kolstad A, Jerkeman M, et al. 15‐year follow‐up of the Second Nordic Mantle Cell Lymphoma trial ( MCL 2): prolonged remissions without survival plateau. Br J Haematol. 2016;175(3):410-418. doi:10.1111/bjh.14241
-
Geisler CH, Kolstad A, Laurell A, et al. Long-term progression-free survival of mantle cell lymphoma after intensive front-line immunochemotherapy with in vivo–purged stem cell rescue: a nonrandomized phase 2 multicenter study by the Nordic Lymphoma Group. Blood. 2008;112(7):2687-2693. doi:10.1182/blood-2008-03-147025
-
Le Gouill S, Thieblemont C, Oberic L, et al. Rituximab after Autologous Stem-Cell Transplantation in Mantle-Cell Lymphoma. N Engl J Med. 2017;377(13):1250-1260. doi:10.1056/NEJMoa1701769
-
Sarkozy C, Thieblemont C, Oberic L, et al. Long-Term Follow-Up of Rituximab Maintenance in Young Patients With Mantle-Cell Lymphoma Included in the LYMA Trial: A LYSA Study. J Clin Oncol. 2024;42(7):769-773. doi:10.1200/JCO.23.01586
-
Silkenstedt E, Dreyling M. First Line Therapy in Mantle Cell Lymphoma—The Role of BTKi in the Initial Treatment of Transplant‐Eligible and ‐Ineligible Patients. Hematological Oncology. 2025;43(S2):e70073. doi:10.1002/hon.70073
-
Dreyling M, Doorduijn J, Giné E, et al. Ibrutinib combined with immunochemotherapy with or without autologous stem-cell transplantation versus immunochemotherapy and autologous stem-cell transplantation in previously untreated patients with mantle cell lymphoma (TRIANGLE): a three-arm, randomised, open-label, phase 3 superiority trial of the European Mantle Cell Lymphoma Network. The Lancet. 2024;403(10441):2293-2306. doi:10.1016/S0140-6736(24)00184-3
-
Wang M, Salek D, Belada D, et al. Acalabrutinib Plus Bendamustine-Rituximab in Untreated Mantle Cell Lymphoma. J Clin Oncol. 2025;43(20):2276-2284. doi:10.1200/JCO-25-00690
-
Wang ML, Jurczak W, Jerkeman M, et al. Ibrutinib plus Bendamustine and Rituximab in Untreated Mantle-Cell Lymphoma. N Engl J Med. 2022;386(26):2482-2494. doi:10.1056/NEJMoa2201817
-
Wang M, Paludo J, de Holanda Farias JS, et al. Time to third-line treatment after bendamustine-rituximab with or without acalabrutinib in patients with previously untreated mantle cell lymphoma: Updated analysis of the phase 3 ECHO trial after 50 months of follow-up. Abstract to be presented at: American Society of Hematology Annual Meeting December 6-9, 2025; Orlando, FL.
-
Jain P, Young Ok C, Nastoupil LJ, et al. Acalabrutinib with Rituximab As First-Line Therapy for Older Patients with Mantle Cell Lymphoma - a Phase II Clinical Trial. Blood. 2023;142(Supplement 1):3036-3036. doi:10.1182/blood-2023-181216
-
Kumar A, Soumerai J, Abramson JS, et al. Zanubrutinib, obinutuzumab, and venetoclax for first-line treatment of mantle cell lymphoma with a TP53 mutation. Blood. 2025;145(5):497-507. doi:10.1182/blood.2024025563
-
Kumar A, Sha F, Toure A, et al. Patterns of survival in patients with recurrent mantle cell lymphoma in the modern era: progressive shortening in response duration and survival after each relapse. Blood Cancer J. 2019;9(6):50. doi:10.1038/s41408-019-0209-5
-
Vose JM, Fu K, Wang L, et al. Integrative analysis of clinicopathological features defines novel prognostic models for mantle cell lymphoma in the immunochemotherapy era: a report from The North American Mantle Cell Lymphoma Consortium. J Hematol Oncol. 2023;16(1):122. doi:10.1186/s13045-023-01520-7
-
Martin P, Cohen JB, Wang M, et al. Treatment Outcomes and Roles of Transplantation and Maintenance Rituximab in Patients With Previously Untreated Mantle Cell Lymphoma: Results From Large Real-World Cohorts. J Clin Oncol. 2023;41(3):541-554. doi:10.1200/JCO.21.02698
-
Fenske TS, Wang XV, Till BG, et al. Lack of Benefit of Autologous Hematopoietic Cell Transplantation (auto-HCT) in Mantle Cell Lymphoma (MCL) Patients (pts) in First Complete Remission (CR) with Undetectable Minimal Residual Disease (uMRD): Initial Report from the ECOG-ACRIN EA4151 Phase 3 Randomized Trial. Blood. 2024;144(Supplement 2):LBA-6-LBA-6. doi:10.1182/blood-2024-212973